Viscoelastic Janus Nanocomposite Hydrogel for Periodontitis Immunomodulation via Co-delivery of IL- 1β Monoclonal Antibody and PDLSC Exosomes
- Department of Periodontology, Peking University School and Hospital of Stomatology & National Center for Stomatology & National Clinical Research Center for Oral Diseases & National Engineering Research Center of Oral Biomaterials and Digital Medical Devices, Beijing, 100081, China
- National Research Institute for Family Planning National Human Genetic Resources Centers, Beijing, 100081, China
- Department of Cell Biology, School of Basic Medical Sciences, Peking University Stem Cell Research Center, Peking University Health Science Center, Peking University, Beijing 100191, China
- First Clinical Division, Peking University School and Hospital of Stomatology & National Center for Stomatology & National Clinical Research Center for Oral Diseases & National Engineering Research Center of Oral Biomaterials and Digital Medical Devices, Beijing, 100034, China

Received: 19-10-2025
Revised: 16-12-2025
Accepted: 28-02-2026
Published in Issue 30-04-2026
Copyright (c) 2026 Lingyan Peng, Guohong Yuan, Jingru Zhao, Xiaohui Yin, Sicong Jiang, Xiangying Ouyang, Jing Qiao (Author)

This work is licensed under a Creative Commons Attribution 4.0 International License.
How to Cite
PDF views: 7
Abstract
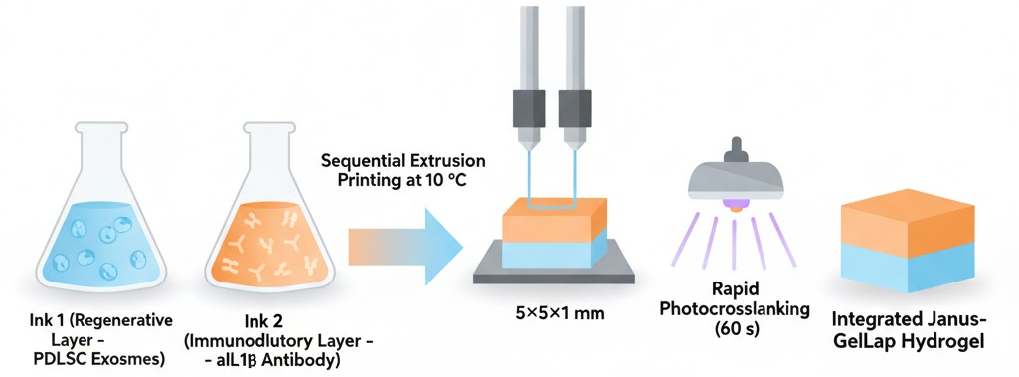
A viscoelastic Janus nanocomposite hydrogel (Janus-GelLap) was engineered via sequential 3D printing using Gelatin Methacryloyl (GelMA) and exfoliated Laponite nanosilicates to enable spatiotemporally controlled co-delivery of a neutralizing IL-1β monoclonal antibody with documented cross-reactivity to rodent IL-1β (aIL1β) and periodontal ligament stem cell-derived exosomes (PDLSC-Exos). The fully exfoliated Laponite network increased the hydrogel’s surface area from 4.85 to 25.84 m²/g and enhanced the storage modulus (G′) from 2.15 to 8.24 kPa, endowing excellent shear-thinning and >95% rapid self-healing. In vitro release studies showed a biphasic diffusion of aIL1β (22 ± 3% burst, 78 ± 4% total) and a sustained zero-order-like release of PDLSC-Exos (61 ± 5% total) over 14 days, governed by Fickian (n = 0.48) and non-Fickian (n = 0.78) mechanisms, respectively. Cytocompatibility tests confirmed >95% cell viability with a 1.3-fold increase in hPDLSC proliferation. In LPS-stimulated macrophages, Janus-GelLap reduced TNF-α and iNOS expression by >80% while elevating Arg-1 and IL-10 by ≈5-fold; ELISA revealed TNF-α = 410 ± 65 pg/mL and IL-10 = 615 ± 80 pg/mL, confirming synergistic M1 suppression and M2 activation. In a rat periodontitis model, micro-CT analysis demonstrated near-complete bone preservation (CEJ–ABC = 0.51 ± 0.06 mm; BV/TV = 68.1 ± 4.6%; BMD = 1.10 ± 0.10 g/cm³; Tb.Th = 85 ± 6 μm), statistically indistinguishable from healthy controls. Although comprehensive periodontal immune cell profiling by flow cytometry and expanded leukocyte panels was not performed, immunofluorescence/immunohistochemistry of the defect region provided direct in vivo evidence of immunomodulation, revealing a pronounced shift in macrophage polarization from F4/80⁺iNOS⁺ M1 to F4/80⁺CD206⁺/Arg-1⁺ M2 phenotypes, accompanied by reduced IL-1β/TNF-α and enhanced OCN/Runx2 expression. These findings establish the Janus-GelLap as a multifunctional immuno-regenerative platform that effectively halts inflammation-driven alveolar bone loss and promotes coordinated tissue regeneration, providing a clinically translatable paradigm for osteoimmunomodulatory therapy in chronic inflammatory diseases such as periodontitis.
Keywords
- Dual drug release,
- Macrophage polarization,
- Nanostructured biomaterial,
- Osteoregeneration,
- Sequential bioprinting
References
- Cheng, R., Wu, Z., Li, M., Shao, M., Hu, T. Interleukin-1β is a potential therapeutic target for periodontitis: a narrative review. Int J Oral Sci 12, 2 (2020).
- Wu, Q., Zhang, W., Lu, Y., Li, H., Yang, Y., Geng, F., Liu, J., Lin, L., Pan, Y., Li, C. Association between periodontitis and inflammatory comorbidities: The common role of innate immune cells, underlying mechanisms and therapeutic targets. Int Immunopharmacol 128, 111558 (2024).
- Radu, C.-M., Radu, C. C., Arbănaşi, E.-M., Hogea, T., Murvai, V. R., Chiș, I.-A., Zaha, D. C. Exploring the efficacy of novel therapeutic strategies for periodontitis: A literature review. Life 14, 468 (2024).
- Rosa, A. C., Mio, M., Andreadou, I., Sumbayev, V. V. Editorial: The challenge of new therapeutic approaches for unmet therapeutic needs. Front Pharmacol 11, 01341 (2020).
- Papathanasiou, E., Conti, P., Carinci, F., Lauritano, D., Theoharides, T. C. IL-1 superfamily members and periodontal diseases. J Dent Res 99, 1425–1434 (2020).
- Han, N., Liu, Y., Du, J., Xu, J., Guo, L., Liu, Y. Regulation of the host immune microenvironment in periodontitis and periodontal bone remodeling. Int J Mol Sci 24, 3158 (2023).
- Goh, A. X., Bertin-Maghit, S., Ping Yeo, S., Ho, A., Derks, H., Mortellaro, A., Wang, C.-I. A novel human anti-interleukin-1β neutralizing monoclonal antibody showing in vivo efficacy. mAbs 6, 764–772 (2014).
- Zhao, D.-Z., Yang, R.-L., Wei, H.-X., Yang, K., Yang, Y.-B., Wang, N.-X., Zhang, Q., Chen, F., Zhang, T. Advances in the research of immunomodulatory mechanism of mesenchymal stromal/stem cells on periodontal tissue regeneration. Front Immunol 15, 1449411 (2025).
- Ahmad, P., Estrin, N., Farshidfar, N., Zhang, Y., Miron, R. J. Mechanistic insights into periodontal ligament stem cell-derived exosomes in tissue regeneration. Clin Oral Investig 29, 357 (2025).
- Bezerra, B., Monajemzadeh, S., Silva, D., Pirih, F. Q. Modulating the immune response in periodontitis. Front Dent Med 3, 879131 (2022).
- Liu, C., Yu, Q., Yuan, Z., Guo, Q., Liao, X., Han, F., Feng, T., Liu, G., Zhao, R., Zhu, Z., Mao, H., Zhu, C., Li, B. Engineering the viscoelasticity of gelatin methacryloyl (GelMA) hydrogels via small “dynamic bridges” to regulate BMSC behaviors for osteochondral regeneration. Bioact Mater 25, 445–459 (2022).
- Andrade, D. B., Soares, L. L. S., Cardoso, F. L. A., Lima, I. S., Silva, J. G. V., Carvalho, M. A. M., Fonseca, M. G., Brito, G. de C., Santos, F. E. P., Osajima, J. A., Lobo, A. O., Silva-Filho, E. C. Hydrogel based on nanoclay and gelatin methacrylate polymeric matrix as a potential osteogenic application. J Funct Biomater 14, 74 (2023).
- Wu, C.-J., Gaharwar, A. K., Chan, B. K., Schmidt, G. Mechanically tough Pluronic F127/Laponite nanocomposite hydrogels from covalently and physically cross-linked networks. Macromolecules 44, 8215–8224 (2011).
- Zhang, S., Jia, Y., Liu, J., Feng, F., Wei, Z., Zhang, M., Xu, F. A viscoelastic alginate-based hydrogel network coordinated with spermidine for periodontal ligament regeneration. Regen Biomater 10, rbad009 (2023).
- Zhang, S., Liu, J., Feng, F., Jia, Y., Xu, F., Wei, Z., Zhang, M. Rational design of viscoelastic hydrogels for periodontal ligament remodeling and repair. Acta Biomater 174, 69–90 (2024).
- Guo, W., Mirzaei, M., Nie, L. Janus hydrogels: Design, properties, and applications. Gels 11, 717 (2025).
- Yan, T., Cheng, J., Liu, H., Wang, Y., Zhang, C., Huang, D., Liu, J., Wang, Z. Multifunctional Janus hydrogels: Surface design strategies for next-generation clinical solutions. Gels 11, 343 (2025).
- Yoon, M. S., Lee, J. M., Jo, M. J., Kang, S. J., Yoo, M. K., Park, S. Y., Bong, S., Park, C.-S., Park, C.-W., Kim, J.-S., Han, S.-B., Lee, H. J., Shin, D. H. Dual-drug delivery systems using hydrogel–nanoparticle composites: Recent advances and key applications. Gels 11, 520 (2025).
- Ayala-Mar, S., Jeon, O., Chacón-Ponce, P., González-Valdez, J., Alsberg, E. Photocrosslinkable and biodegradable hydrogels for the controlled delivery of exosomes. bioRxiv (2025), 2025–04.
- Chen, M., Zhao, X., Liu, Y. Dry and cool: A Janus coated textile for simultaneous radiative cooling and unidirectional sweat transport. Prog Org Coat 211, 109794 (2026).
- Zhang, Y., Zhang, M., Li, Y., Liu, J., Liu, K., Xu, Y., Lan, Y., Zeng, Y. Janus fiber-based membrane for humid condition filtration with concurrent air filtration and directional water transport. ACS Appl Mater Interfaces (2026), in press.
- Jiang, Y., Zhu, C., Ma, X., Fan, D. Janus hydrogels: Merging boundaries in tissue engineering for enhanced biomaterials and regenerative therapies. Biomater Sci 12, 2504–2520 (2024).
- Zhang, Y., Chen, Y., Ding, T., Zhang, Y., Yang, D., Zhao, Y., Liu, J., Ma, B., Bianco, A., Ge, S., Li, J. Janus porous polylactic acid membranes with versatile metal–phenolic interface for biomimetic periodontal bone regeneration. npj Regen Med 8, 28 (2023).
- Yang, D., Xu, Z., Huang, D., Luo, Q., Zhang, C., Guo, J., Tan, L., Ge, L., Mu, C., Li, D. Immunomodulatory multifunctional Janus collagen-based membrane for advanced bone regeneration. Nat Commun 16, 4264 (2025).
- Liu, T., Hu, W., Zou, X., Xu, J., He, S., Chang, L., Li, X., Yin, Y., Tian, M., Li, Z., Zhou, J., Jiang, X., Chen, S. Human periodontal ligament stem cell-derived exosomes promote bone regeneration by altering microRNA profiles. Stem Cells Int 2020, 8852307 (2020).
- Shi, C., Wu, Z., Li, Y., Zhang, X., Xu, Y., Chen, A., Yan, C., Shi, Y., Wang, T., Su, B. Superhydrophobic/superhydrophilic Janus evaporator for extreme high salt-resistance solar desalination by an integrated 3D printing method. ACS Appl Mater Interfaces 15, 23971–23979 (2023).
- Xie, Y., Guan, Q., Guo, J., Chen, Y., Yin, Y., Han, X. Hydrogels for exosome delivery in biomedical applications. Gels 8, 328 (2022).
- Wu, J.-Y., Li, Y.-J., Hu, X.-B., Huang, S., Xiang, D.-X. Preservation of small extracellular vesicles for functional analysis and therapeutic applications: A comparative evaluation of storage conditions. Drug Deliv 28, 162–170 (2021).
- Zhang, W., Chen, R., Xu, X., Zhu, L., Liu, Y., Yu, X., Tang, G. Construction of biocompatible hydrogel scaffolds with a long-term drug release for facilitating cartilage repair. Front Pharmacol 13, 922032 (2022).
- Zhang, L., Nie, F., Zhao, J., Li, S., Liu, W., Guo, H., Yang, P. PGRN is involved in macrophage M2 polarization regulation through TNFR2 in periodontitis. J Transl Med 22, 407 (2024).
- Pucinelli, C. M., Nelson-Filho, P., Lucisano, M. P., León, J. E., Faccioli, L. H., Sorgi, C. A., Silva, C. M. P. C., da Silva, L. A. B., da Silva, R. A. B. M1 and M2 macrophages markers are alternately expressed during periapical lesion development. J Appl Oral Sci 33, e20240579 (2025).
- Wang, T., Zhu, Z., Hua, W., Xue, S. Immunomodulatory potential of a composite amniotic membrane hydrogel for wound healing: Effects on macrophage cytokine secretion. Biomedicines 13, 2574 (2025).
- Chen, J., Guan, X., Chen, L., Zheng, B., Li, F., Fang, C., Fu, Y., Li, X., Wang, H., Zhou, Y. Customized hydrogel system for the spatiotemporal sequential treatment of periodontitis propelled by ZEB1. Adv Sci (Weinh) 12, 2503338 (2025).
- Wang, Y., Jin, S., Guo, Y., Lu, Y., Deng, X. Adhesive and injectable hydrogel microspheres for NRF2-mediated periodontal bone regeneration. Int J Oral Sci 17, 7 (2025).
- Albougha, M. S., Sugii, H., Adachi, O., Mardini, B., Soeno, S., Hamano, S., Hasegawa, D., Yoshida, S., Itoyama, T., Obata, J., Maeda, H. Exosomes from human periodontal ligament stem cells promote differentiation of osteoblast-like cells and bone healing in rat calvarial bone. Biomolecules 14, 1455 (2024).
- Li, W., Wang, Z., Jiang, L., Feng, M., Fan, X., Fan, H., Xiang, J. A facile synthetic approach to UV-degradable hydrogels. Polymers 15, 3762 (2023).
- Zhou, L., Zhang, C., Shi, T., Wu, D., Chen, H., Han, J., Chen, D., Lin, J., Liu, W. Functionalized 3D-printed GelMA/Laponite hydrogel scaffold promotes BMSCs recruitment through osteoimmunomodulatory enhance osteogenic via AMPK/mTOR signaling pathway. Mater Today Bio 29, 101261 (2024).
- Liu, B., Li, J., Lei, X., Miao, S., Zhang, S., Cheng, P., Song, Y., Wu, H., Gao, Y., Bi, L., Pei, G. Cell-loaded injectable gelatin/alginate/LAPONITE® nanocomposite hydrogel promotes bone healing in a critical-size rat calvarial defect model. RSC Adv 10, 25652–25661 (2020).
- Andrade, D. B., Soares, L. L. S., Cardoso, F. L. A., Lima, I. S., Silva, J. G. V., Carvalho, M. A. M., Fonseca, M. G., Brito, G. de C., Santos, F. E. P., Osajima, J. A., Lobo, A. O., Silva-Filho, E. C. Hydrogel based on nanoclay and gelatin methacrylate polymeric matrix as a potential osteogenic application. J Funct Biomater 14, 74 (2023).
- Andrade, D. B., Soares, L. L. S., Cardoso, F. L. A., Lima, I. S., Silva, J. G. V., Carvalho, M. A. M., Fonseca, M. G., Brito, G. de C., Santos, F. E. P., Osajima, J. A., Lobo, A. O., Silva-Filho, E. C. Hydrogel based on nanoclay and gelatin methacrylate polymeric matrix as a potential osteogenic application. J Funct Biomater 14, 74 (2023).
- Yang, Y., He, L., Guan, G., Xu, S., Ge, W., Liu, J., Xie, X., Lei, L. Janus hydrogels: Pioneering dual-faced biomaterials for revolutionary tissue engineering. Mater Today Adv 28, 100652 (2025).
- Zhang, R., Zhang, M., Chen, L., Jiang, L., Zou, C., Li, N., Zhou, H., Feng, S. Dual-phase SilMA hydrogel: A dynamic scaffold for sequential drug release and enhanced spinal cord repair via neural differentiation and immunomodulation. Front Bioeng Biotechnol 12, 1501488 (2024).
- Tu, K., Wu, J., Zhu, W. Fabrication and characterization of novel macroporous hydrogels based on the polymerizable surfactant AAc-Span80 and their enhanced drug-delivery capacity. RSC Adv 12, 29677–29687 (2022).
- Matshitse, R. Brunauer-Emmett-Teller (BET) surface area analysis. Rhodes Univ Natl Res Found 384 (2010).
- Davern, J. W., Hipwood, L., Bray, L. J., Meinert, C., Klein, T. J. Addition of Laponite to gelatin methacryloyl bioinks improves the rheological properties and printability to create mechanically tailorable cell culture matrices. APL Bioeng 8, 016101 (2024).
- Zhang, L., He, G., Yu, Y., Zhang, Y., Li, X., Wang, S. Design of biocompatible chitosan/polyaniline/Laponite hydrogel with photothermal conversion capability. Biomolecules 12, 1089 (2022).
- Michaelides, K., Al Tahan, M. A., Zhou, Y., Trindade, G. F., Cant, D. J., Pei, Y., Dulal, P., Al-Khattawi, A. A. New insights on the burst release kinetics of spray-dried PLGA microspheres. Mol Pharm 21, 6245–6256 (2024).
- Nikravesh, N., Davies, O. G., Azoidis, I., Moakes, R. J. A., Marani, L., Turner, M., Kearney, C. J., Eisenstein, N. M., Grover, L. M., Cox, S. C. Physical structuring of injectable polymeric systems to controllably deliver nanosized extracellular vesicles. Adv Healthc Mater 8, 1801604 (2019).
- Hwang, H. S., Lee, C.-S. Exosome-integrated hydrogels for bone tissue engineering. Gels 10, 762 (2024).
- Ju, Y., Hu, Y., Yang, P., Xie, X., Fang, B. Extracellular vesicle-loaded hydrogels for tissue repair and regeneration. Mater Today Bio 18, 100522 (2023).
- Chen, S., Saeed, A. F. U. H., Liu, Q., Jiang, Q., Xu, H., Xiao, G. G., Rao, L., Duo, Y. Macrophages in immunoregulation and therapeutics. Signal Transduct Target Ther 8, 207 (2023).
- Arora, S., Dev, K., Agarwal, B., Das, P., Syed, M. A. Macrophages: Their role, activation and polarization in pulmonary diseases. Immunobiology 223, 383–396 (2018).
- Zhang, X., Tian, X., Wang, Y., Yan, Y., Wang, Y., Su, M., Lv, H., Li, K., Hao, X., Xing, X., Song, S. Application of lipopolysaccharide in establishing inflammatory models. Int J Biol Macromol 279, 135371 (2024).
- Wichienrat, W., Surisaeng, T., Sa-Ard-Iam, N., Chanamuangkon, T., Mahanonda, R., Wisitrasameewong, W. Alveolar bone loss in a ligature-induced periodontitis model in rat using different ligature sizes. Eur J Dent 18, 933–941 (2024).
- Gui, Y., Zhang, Y., Xu, H., Yang, W., Huang, H., Gu, M., Sun, Y. Recent advances in hydrogels for treating periodontal diseases and oral mucosal diseases. Front Bioeng Biotechnol 13, 1605672 (2025).
- Shen, Z., Kuang, S., Zhang, Y., Yang, M., Qin, W., Shi, X., Lin, Z. Chitosan hydrogel incorporated with dental pulp stem cell-derived exosomes alleviates periodontitis in mice via a macrophage-dependent mechanism. Bioact Mater 5, 1113–1126 (2020).
- Qiao, X., Tang, J., Dou, L., Yang, S., Sun, Y., Mao, H., Yang, D. Dental pulp stem cell-derived exosomes regulate anti-inflammatory and osteogenesis in periodontal ligament stem cells and promote the repair of experimental periodontitis in rats. Int J Nanomedicine 18, 4683–4703 (2023).
- Nakao, Y., Fukuda, T., Zhang, Q., Sanui, T., Shinjo, T., Kou, X., Chen, C., Liu, D., Watanabe, Y., Hayashi, C., Yamato, H., Yotsumoto, K., Tanaka, U., Taketomi, T., Uchiumi, T., Le, A. D., Shi, S., Nishimura, F. Exosomes from TNF-α-treated human gingiva-derived MSCs enhance M2 macrophage polarization and inhibit periodontal bone loss. Acta Biomater 122, 306–324 (2021).
- Lee, Y.-K., Wadhwa, P., Cai, H., Jung, S.-U., Zhao, B. C., Rim, J.-S., Kim, D.-H., Jang, H.-S., Lee, E.-S. Micro-CT and histomorphometric study of bone regeneration effect with autogenous tooth biomaterial enriched with platelet-rich fibrin in an animal model. Scanning 2021, 6656791 (2021).
- Zhao, P., Li, M., Wang, J., Li, J., Lin, Y. Targeting the immune microenvironment: A novel strategy for treating infected bone defects with hydrogels. Chin Chem Lett 36, 111319 (2025).

 10.57647/jnsc.2026.1602.07
10.57647/jnsc.2026.1602.07